What Should the Next Assistant Secretary for SAMSHA Be and Do to Heal America Psyche?
February 04, 2021
February 04, 2021
America doesn’t feel so good in body, mind, or spirit—from children through seniors. America’s mental health was fragile before COVID-19, carefully laid out in multiple Institute of Medicine Reports authored by my colleagues [1], and the in-our-face Opioid and Suicide Epidemics. And, then, there is simmering violence in America.
The COVID-19 epidemic made our physical, mental and spiritual health much worse for the last year. Even before COVID and the election, American’s mental, emotional, and behavioral well-being was compromised. I could spend days writing about the underlying epidemiology of all this mental, emotional, and behavioral suffering. Just a few Post-It Notes make the point:
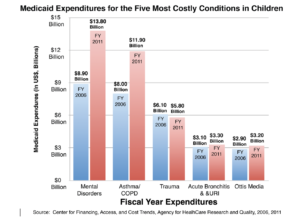
The above data were from about a decade ago, and the situation is worse today, both for children and adults. Meanwhile, we’ve gone through a decade of the Opiate epidemic, which was not a good self-help way to deal with the mental, emotional, and behavioral health problems ripping the heartlands of America. Sadly, SAMHSA did not widely fund the most cost-effective treatment strategy supported by the National Institute on Drug Abuse (NIDA), the work of the late brilliant scientist whose work was funded by NIDA and scalable to any community in America [5-8]. Good science is more important than status or political party. I don’t give a damn about my oncologist’s politics; I care about how good that doctor is, and she is damn good. I’m 14 years OK.
How important is that scientifically proven strategy for serious substance abuse and mental health in the middle of the COVID virus? Very. That simple contingency-management protocol can be used anywhere, as recommended by the International Society of Addiction Medicine Practice and Policy Interest Group Position Paper [9]. It can and does work in inner cities with historic disparities, in West Virginia’s hallows, on Tribal lands in Arizona, or even in small-town middle America where I was born. It can even be done remotely. That is excellent news, and it is ridiculously cheap to implement—and could even be promoted on TV, which did in Pima County, Arizona for Meth [10]. There are similar, well-proven yet straightforward strategies and low-cost to mitigate or treat serious mental illness—yet not widely used across America [11-14].
How important is child-maltreatment in the middle of Covid? Huge. Yet, we will not be able to treat our way out with one-to-one therapy or home visits. But the randomized control study that prevented child-maltreatment at a population level was not therapy; rather, it was the promotion of simple—yet well-proven—strategies that families could adopt and use from the media and brief interactions [15]. An extraordinary study in the United Kingdom indicated population-level improvements in parenting via an eight-week TV show [16], using the same strategies in a CDC-funded study to reduce child maltreatment at a population level of US$7 per child [17].
It’s not just an epidemic of addictions that the new SAMSHA Assistant Secretary must address. We also have had an epidemic of mental illnesses. A regular human might apprehend that something is wrong in America, by the volume of TV ads for psychotropic medications that also are costly and with frequent serious adverse effects even for the most common adult psychiatric disorder of depression [18]. Amazingly, it is possible to use a TV show to reduce depression at a population level [19].
Covid is very likely to have a terrible effect on both mental and physical health, not just now but also over time. Why? Plunging poverty and loss of social connections [20] since the start of the epidemic. Depression rates, for example, are 4.5 times higher for folks well-below the poverty level [20]. Many people in America have moved into deep poverty since Covid.
Of course, we need to heal the national malaise from physical effects COVID. That’s Dr. Fauci’s and the new Surgeon General’s job, and both have the street cred to do so. That’s not enough, though. Collectively, as a people, we are alternating between numbness, fear about health, safety and money; and anger with an anxiety with rattling thoughts that the virus may never go away. We also need improve the historic physical, behavioral and mental harms to people with long-standing disparities—Indigenous peoples, the descendants of slavery, working-class folks who have left behind in the new economy.
The new leadership at SAMSHA must come up with a National “MacGyver” set of strategies that can be implemented in every nook and cranny of American communities to stop the downward slide in mental, emotional, and behavioral health well documented before COVID and significantly worsened since COVID. It will require a national “scoreboard” or “thermometer” for recovering our social, physical, and economic well-being. Some of those scientific principles to do so are well documented in bio, behavioral-medical sciences [21-23].
Of course, we need to heal the national malaise from the physical effects of COVID. That’s Dr. Fauci’s and the new Surgeon General’s job, and both have the street cred to do so. That’s not enough, though. The job of the Assistant Secretary at SAMSHA is for America’s collective mental, emotional, and behavioral health.
As a people, we are collectively alternating between numbness, fear about health, safety, and money, and anger and anxiety with rattling thoughts that the virus may never go away. We also need to improve the historic physical, behavioral and mental harms to people with long-standing disparities—Indigenous peoples, the descendants of slavery, working-class folks who have left behind in the new economy.
Our hydra-headed crises are very complicated and dangerous, with universal economic, mental and physical health collapse for so many in America. It touches every spectrum of life in small towns in middle America like my hometown in Western Kansas, to people in big cities across America and every place in between. All of us have witnessed the tragedy of lost jobs, homelessness, lost health care, and the anxiousness as we struggled for daily necessities, paying rent or mortgage, to making a doctors’ appointment. The trend was there before COVID, and it will be worse post-COVID.
America will need an extraordinary leader and leadership team to prevent, treat, and heal the nation’s mental, emotional, and behavioral health—while we deal with the spiritual and wellness thief of Covid-19. That is the Assistant Secretary of Health and Human Services for Mental Health and Substance (SAMSHA) position. God speed to the new Assistant Secretary. She or he will be very important for the future of America’s mental, physical, and economic well-being when you view the graph of our finances and our well-being.
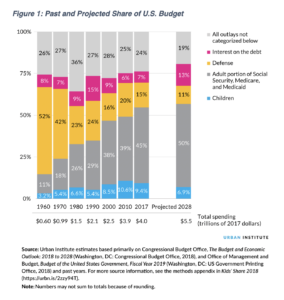
The next Assistant Secretary to run SAMSHA must have the wisdom, knowledge, drive to innovate and create systems of care and delivery to prevent, intervene, and treat mental, emotional, and behavioral disorders—at a population-level scale that can turn around the epidemic. The prevalence rates of depression, for example, have been increasing among every birth cohort for the past several decades.
The new administration must now appoint a new Assistant Secretary when the nation’s mental health among children, adults, families, and communities is now more fragile because of the horrific impact of COVID and the economic downturn. Meanwhile, the issues of opiates, other addictions have remained or appear to be increasing because of loss of employment, safety, medical care, and other disruptions from a year of social isolation, job loss, uncertainty, and down-right fear in the present and future.
The practical, proven science exists in Institute of Medicine Reports and other scientific documents in the National Library of Medicine (www.pubmed.gov) to fast-forward the physical, mental, emotional, and educational wellbeing of America’s peoples for the safety, security, health, and economic wellbeing of our social capital for our futures. SAMSHA funding touches every community in America with the very mission to improve the mental, emotional, and behavioral health of our children and their families as rapidly as possible.
The next Assistant Secretary of SAMSHA must be a potent, scientifically informed servant leader who does more than authorize funding. She, or he, must inspire the SAMSHA staff, the states’ leadership in mental health, and allied entities and advocates—throughout the country—to mobilize rapid improvement of positive indicators of mental and physical health among our children, families, schools, and communities for our nation to recover. The science exists to do so, and it is cheap and scalable.
Are you in or out for the challenge? Let’s find those potent, visionary leaders.

Dr. Embry is an internationally noted prevention scientist and child and developmental psychologist. He is president/senior scientist at PAXIS Institute in Tucson, AZ., the scientific advisor to the Children’s Mental Health Network, and a member of the Advisory Council for the U.S. Center for Mental Health Services.